Hypokalaemia, a condition characterized by abnormally low levels of potassium in the blood, is a common electrolyte imbalance that can have significant implications for cardiac health. One of the critical aspects of managing hypokalaemia is understanding the ECG changes hypokalaemia can cause. These changes are not only diagnostic but also crucial for monitoring the severity of the condition and guiding treatment decisions.
Understanding Hypokalaemia
Hypokalaemia occurs when the serum potassium level falls below 3.5 mmol/L. This condition can be caused by various factors, including:
- Inadequate potassium intake
- Increased potassium excretion due to diuretics or gastrointestinal losses
- Transcellular shifts of potassium into cells
Potassium is essential for maintaining normal cardiac function, and its deficiency can lead to serious cardiac complications, including arrhythmias and even cardiac arrest.
ECG Changes in Hypokalaemia
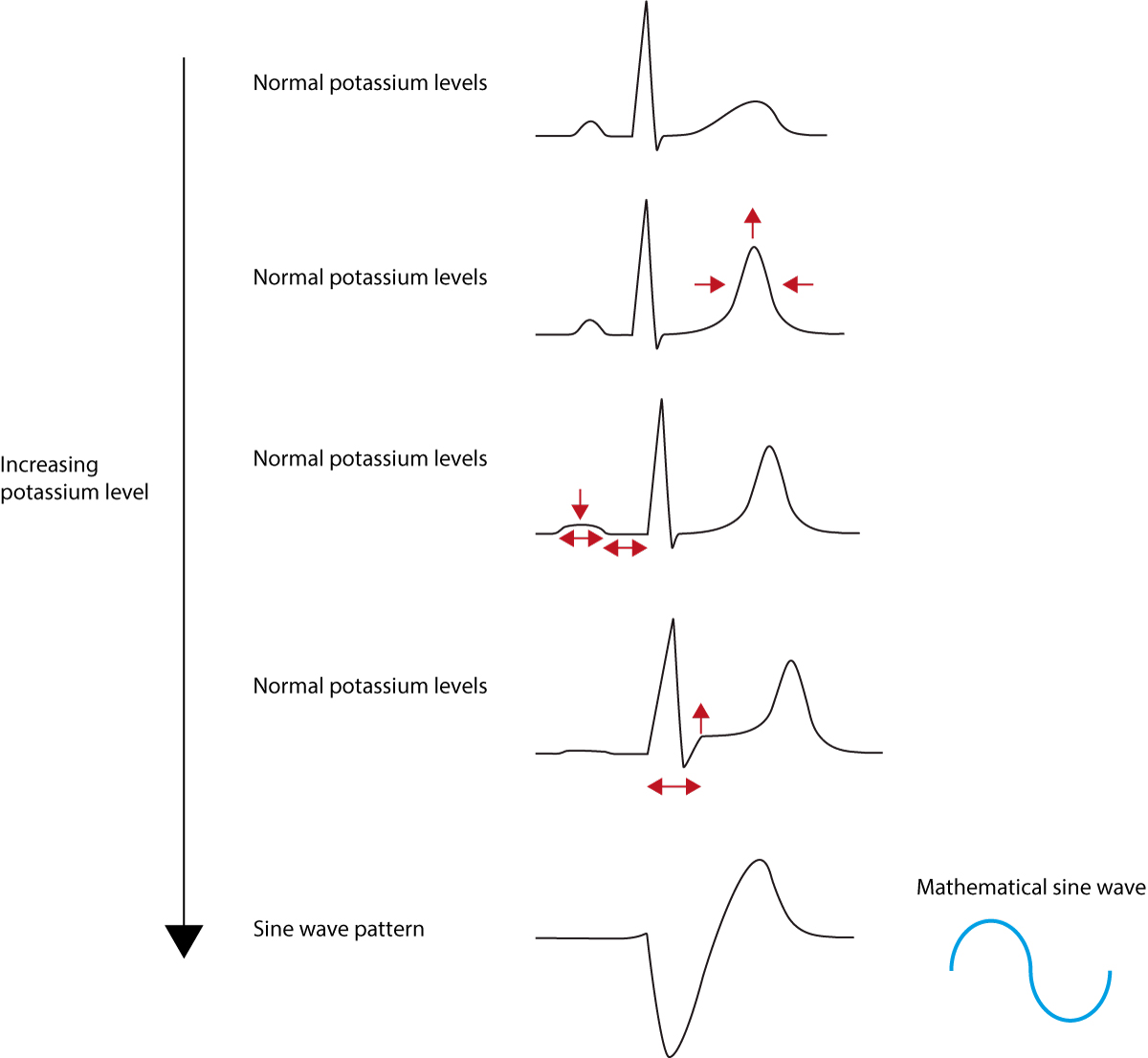
Electrocardiogram (ECG) changes are often the first indicators of hypokalaemia. These changes can vary depending on the severity of the potassium deficiency. The most common ECG changes hypokalaemia include:
- T-wave flattening or inversion: This is often one of the earliest signs of hypokalaemia. The T-waves may become flattened or inverted, particularly in the precordial leads.
- ST-segment depression: Hypokalaemia can cause depression of the ST segment, which may mimic ischemia.
- U-waves: Prominent U-waves, which are small deflections following the T-wave, are a classic sign of hypokalaemia. These waves become more pronounced as the potassium level decreases.
- Prolonged QT interval: The QT interval may be prolonged, increasing the risk of ventricular arrhythmias.
- Arrhythmias: Severe hypokalaemia can lead to various arrhythmias, including atrial fibrillation, ventricular tachycardia, and even ventricular fibrillation.
Severity of ECG Changes
The severity of ECG changes hypokalaemia can be categorized based on the degree of potassium deficiency:
| Potassium Level (mmol/L) | ECG Changes |
|---|---|
| 3.0-3.5 | Mild T-wave flattening or inversion, ST-segment depression |
| 2.5-3.0 | Prominent U-waves, more pronounced T-wave changes |
| 2.0-2.5 | Significant ST-segment depression, prolonged QT interval |
| <2.0 | Severe arrhythmias, including ventricular tachycardia and fibrillation |
Diagnosing Hypokalaemia
Diagnosing hypokalaemia involves a combination of clinical assessment, laboratory tests, and ECG evaluation. The diagnostic process typically includes:
- Clinical history and physical examination: Assessing symptoms such as muscle weakness, cramps, and fatigue, as well as signs of dehydration or gastrointestinal losses.
- Laboratory tests: Measuring serum potassium levels and other electrolytes. Additional tests may include renal function tests and urine potassium levels to determine the cause of hypokalaemia.
- ECG: Performing an ECG to identify characteristic ECG changes hypokalaemia. This is crucial for assessing the cardiac impact of the condition and guiding treatment.
Managing Hypokalaemia
The management of hypokalaemia focuses on correcting the potassium deficiency and addressing the underlying cause. Treatment strategies include:
- Oral potassium supplementation: For mild to moderate hypokalaemia, oral potassium supplements or potassium-rich foods can be used to restore normal potassium levels.
- Intravenous potassium replacement: In severe cases or when oral supplementation is not feasible, intravenous potassium replacement may be necessary. This should be done under close monitoring to avoid complications such as hyperkalemia.
- Addressing the underlying cause: Treating the underlying condition, such as stopping diuretics, managing gastrointestinal losses, or correcting metabolic alkalosis.
- Monitoring: Regular monitoring of serum potassium levels and ECG changes to ensure effective treatment and prevent recurrence.
🔍 Note: Intravenous potassium replacement should be administered with caution, as rapid correction can lead to hyperkalemia and cardiac arrhythmias.
Preventing Hypokalaemia
Preventing hypokalaemia involves maintaining adequate potassium intake and managing conditions that can lead to potassium loss. Key preventive measures include:
- Balanced diet: Consuming a diet rich in potassium, including fruits, vegetables, and whole grains.
- Avoiding excessive diuretic use: Using diuretics judiciously and monitoring potassium levels regularly.
- Managing gastrointestinal conditions: Treating conditions that cause gastrointestinal losses, such as diarrhea or vomiting, promptly.
- Regular monitoring: For individuals at risk of hypokalaemia, regular monitoring of serum potassium levels and ECG changes can help detect and manage the condition early.
Hypokalaemia is a serious condition that requires prompt recognition and management. Understanding the ECG changes hypokalaemia can cause is crucial for early diagnosis and effective treatment. By recognizing the characteristic ECG changes and addressing the underlying cause, healthcare providers can prevent serious complications and improve patient outcomes. Regular monitoring and preventive measures can also help manage hypokalaemia and reduce the risk of recurrence.
Related Terms:
- hypokalaemia u waves ecg
- hypokalemia on ekg shows
- u wave ecg hypokalemia
- ekg changes in hypokalemia
- hypokalaemia nice cks
- ecg changes hypokalaemia litfl