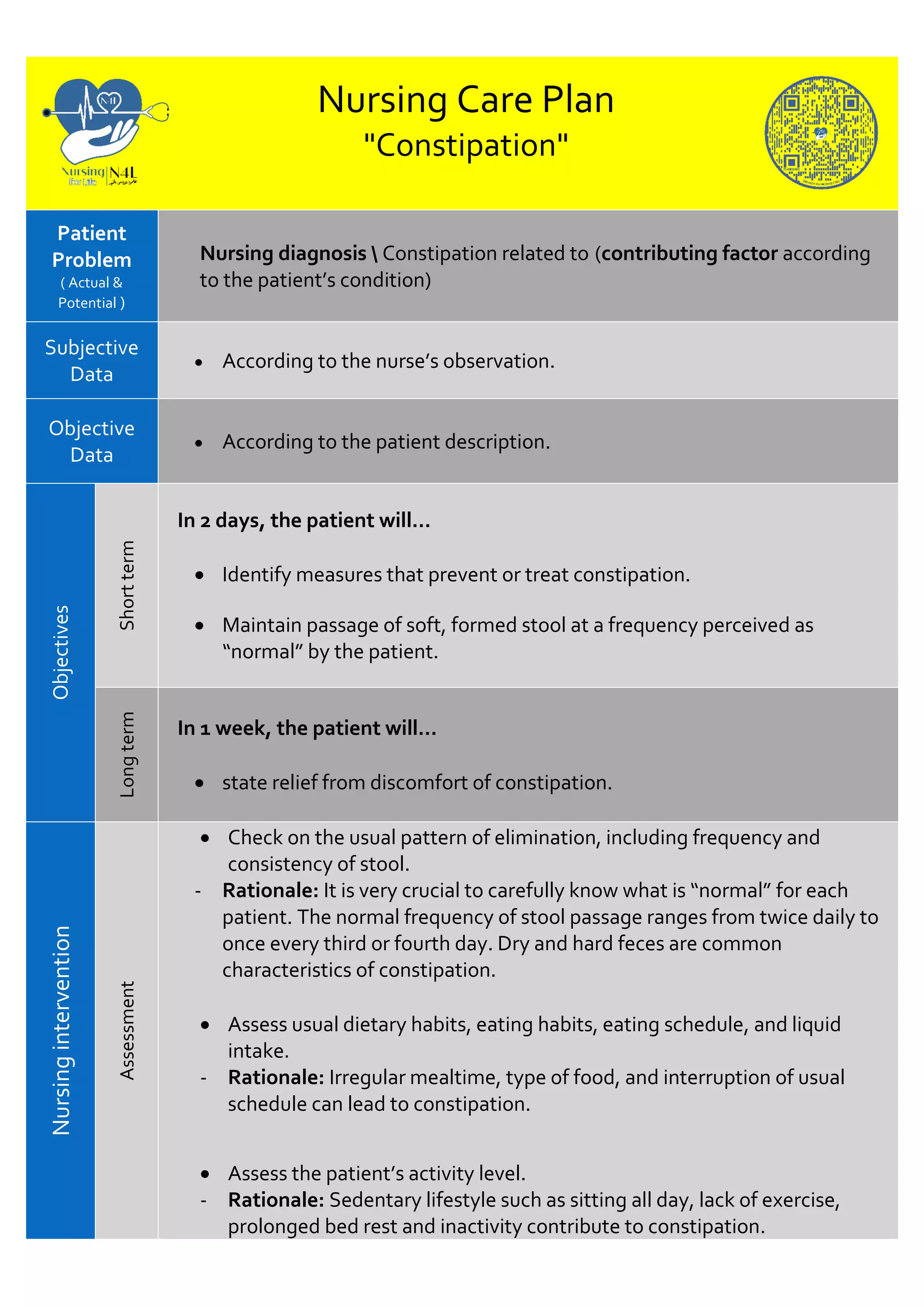
Constipation is a common health issue that affects people of all ages, and it can significantly impact an individual's quality of life. For healthcare professionals, particularly nurses, understanding and managing constipation is crucial. This blog post delves into the intricacies of constipation nursing diagnosis, providing a comprehensive guide on assessment, intervention, and management strategies.
Understanding Constipation
Constipation is characterized by infrequent bowel movements, difficulty passing stools, or a feeling of incomplete evacuation. It can be acute or chronic, with chronic constipation lasting for more than a few weeks. The causes of constipation are varied and can include dietary factors, lack of physical activity, medications, and underlying medical conditions.
Assessing Constipation
Accurate assessment is the first step in managing constipation. Nurses play a pivotal role in this process by conducting a thorough evaluation of the patient’s symptoms, medical history, and lifestyle factors. Key areas to assess include:
- Bowel movement frequency and consistency
- Presence of abdominal pain or discomfort
- Medication use, particularly those known to cause constipation
- Dietary habits, including fiber and fluid intake
- Level of physical activity
- Psychosocial factors, such as stress or anxiety
Constipation Nursing Diagnosis
Once the assessment is complete, nurses can formulate a constipation nursing diagnosis. This diagnosis helps guide the development of an individualized care plan. Common nursing diagnoses related to constipation include:
- Constipation related to decreased mobility
- Constipation related to inadequate fluid intake
- Constipation related to dietary deficiencies
- Constipation related to medication side effects
Intervention Strategies
Interventions for constipation are multifaceted and aim to address the underlying causes. Nurses can implement various strategies to help patients manage constipation effectively. These include:
Dietary Modifications
Encouraging a high-fiber diet is one of the most effective ways to prevent and treat constipation. Nurses should educate patients on the importance of consuming foods rich in fiber, such as fruits, vegetables, whole grains, and legumes. Adequate hydration is also crucial, as it helps soften stools and facilitates easier passage.
Physical Activity
Regular physical activity stimulates bowel movements and helps prevent constipation. Nurses should encourage patients to engage in moderate exercise, such as walking, swimming, or yoga, for at least 30 minutes a day. For patients with mobility issues, gentle exercises or range-of-motion activities can be beneficial.
Medication Management
Certain medications can exacerbate constipation. Nurses should review the patient’s medication list and consult with the healthcare provider to adjust or change medications if necessary. Additionally, laxatives and stool softeners may be prescribed to help relieve constipation. It is essential to educate patients on the proper use of these medications to avoid dependence and other complications.
Behavioral Interventions
Establishing a regular bowel routine can help prevent constipation. Nurses should advise patients to set aside time each day for bowel movements, preferably after a meal when the colon is most active. Creating a comfortable and private environment can also encourage regular bowel movements.
Education and Support
Patient education is a critical component of constipation management. Nurses should provide clear and concise information about constipation, its causes, and management strategies. Offering emotional support and addressing any psychosocial factors contributing to constipation can also enhance patient outcomes.
Monitoring and Evaluation
Ongoing monitoring and evaluation are essential to ensure the effectiveness of the care plan. Nurses should regularly assess the patient’s bowel movements, symptoms, and response to interventions. Adjustments to the care plan may be necessary based on the patient’s progress and any changes in their condition.
📝 Note: Regular follow-up and communication with the healthcare team are crucial for optimal management of constipation.
Special Considerations
Certain patient populations may require special considerations when managing constipation. These include:
Elderly Patients
Elderly patients are at a higher risk of constipation due to age-related changes in the digestive system, decreased mobility, and medication use. Nurses should be particularly vigilant in assessing and managing constipation in this population, focusing on dietary modifications, hydration, and gentle exercises.
Pediatric Patients
Constipation in children can be challenging to manage and may require a different approach. Nurses should educate parents on the importance of a high-fiber diet, adequate hydration, and regular physical activity. Behavioral interventions, such as establishing a regular bowel routine, can also be beneficial.
Patients with Chronic Conditions
Patients with chronic conditions, such as diabetes, neurological disorders, or gastrointestinal diseases, may have unique challenges related to constipation. Nurses should work closely with the healthcare team to develop an individualized care plan that addresses the specific needs of these patients.
Preventing Constipation
Prevention is always better than cure. Nurses can play a proactive role in preventing constipation by educating patients on healthy lifestyle habits. Key preventive measures include:
- Consuming a high-fiber diet
- Staying hydrated
- Engaging in regular physical activity
- Avoiding prolonged periods of inactivity
- Managing stress and anxiety
By promoting these healthy habits, nurses can help patients maintain regular bowel movements and reduce the risk of constipation.
Constipation is a common yet manageable condition that significantly impacts an individual’s quality of life. Nurses, with their comprehensive assessment skills and holistic approach to care, are well-positioned to address constipation nursing diagnosis effectively. Through a combination of dietary modifications, physical activity, medication management, behavioral interventions, and patient education, nurses can help patients achieve and maintain regular bowel movements. Ongoing monitoring and evaluation, along with special considerations for specific patient populations, ensure that the care plan remains effective and tailored to the individual’s needs. By focusing on prevention and early intervention, nurses can play a crucial role in improving patient outcomes and enhancing their overall well-being.
Related Terms:
- nursing implications for constipation
- constipation nursing diagnosis examples
- nursing diagnosis for bowel elimination
- nursing diagnosis for bowel obstruction
- constipation nursing care plan goals
- nursing diagnosis for fecal impaction